The Transformation of Hospitals in a Digital World
The digital transformation of Healthcare in Latin America: a passing fad or a change of mindset to think in a digital way?


Article published in América Economía
Digital transformation is a recurring theme in both general and specialized media all over the world. All sectors of the economy and society are being impacted, to a greater or lesser extent, by a wave of transformative change that all of the major newspapers, magazines and information websites around the world are talking about. Of course, digital transformation has also reached the hospital sector, sometimes even without the actors themselves being terribly aware of the impact and depth of the coming changes. In this regard, we need to understand the real dimension of the concept of digital transformation.
The digital transformation process is not about computerizing a hospital, making Apps, making it easier for patients to make appointments online, letting the clinical and administrative staff to use their own smartphones or tablets, or opening a Facebook or Twitter account for the hospital. While these elements may be part of a transformational process, we cannot reduce the transformation to the use of a specific technology or mix up form and content.
Digital transformation is a continuous, complex and multidimensional process that is linked to social, economic and technological factors that go beyond the hospital walls. It impacts the very essence of what we are and what we do. The real first step a hospital administrator should take is to fully understand that we are not talking about a fad or “something that needs to be installed”; we are talking about a change of mindset with regard to hospital processes, and to start thinking in digital terms. Undoubtedly, the best starting point seems obvious: putting the patient at the center of this transformation.
The Patient at the Center
Hospitals and the healthcare industry in general, currently live in their own two-speed world: On the one hand, is the unstoppable growth and modernization of medical procedures and diagnostic techniques (including the automation of some truly complex procedures); the amazing advances in clinical use materials (some of them generated by 3D printers), or the use of smart drugs or gene therapy. This contrasts sharply with traditional and bureaucratic organizational methods, or the generally slow and inflexible business processes, that in most cases, are isolated and disconnected from their outside reality.
Even the most modern hospitals, with futuristic architecture, sophisticated equipment, and an interest in modern management concepts, seem to walk with feet of clay when seen from a digital transformation perspective. It seems that the administrators of these hospitals have taken short cuts, buying a new technological suit to dress up the old 19th century processes, without actually thinking about the nature and the raison d’etre of the organization, with an eye on the 21st century.
It is important to remember that hospitals exist in order to treat patients, who sometimes feel like they are on a production line in these healthcare organizations, made to serve more the internal functions of the institution, rather than taking note of the needs and expectations of the patient.
This is why the true digital transformation of hospitals must begin with the understanding of the patients in their entirety, beginning of course, with the ailments that brought them here (or better yet, preventing their arrival), but also with their contexts, lifestyles, their habits, their families and social environments. Understand also that the patient is and will increasingly be an active digital subject, with access to technologies that can and should be used as an integral and natural part of the care process and monitoring.
Healthcare organizations should really look at the patient and organize themselves to give efficient and effective care, from the human and from the technical perspectives.
Technology, rather than distance, can and must humanize the “encounters” and facilitate patient-physician exchange through safe communication and doctor-patient confidentiality.
Of course, patients want and demand that their information is used fully and intelligently. There is nothing more frustrating and irrational for the citizen/patient in the world today, than to recite their personal and family medical history again and again, even in the same hospital. Disintegrated data is a recurring problem throughout all of Latin America, from the lack of integration inside the same hospital, or between the hospital and healthcare area, not to mention the higher administrative and geographical levels (municipal, provincial, national, international).
If we could connect the large amount of data produced by healthcare organizations, and connect them intelligently with the data that the patient possess, or that other public or private entities may share about the social, economic and natural environments that the patient is immersed in, we could carry out extraordinarily different and exponentially more effective management than we do today.
The Great Predictive Wave
In this regard, the predictive ability of intelligent algorithms will be a source of disruptive innovation for the hospital sector, both in terms of clinical processes, and administrative and economic management of the hospital sector.
A study carried out by ehCOS and NTTDATA NEXT, the largest database of startups in the world, on trends in Artificial Intelligence in the healthcare field, offers us revealing data about this predictive wave: more than 5 billion dollars invested in emerging companies in this promising field.
Such is the interest in this emerging segment, that a survey conducted by Silicon Valley Bank on more than 120 executives of health technology companies showed that Artificial Intelligence programs, Big Data applied to the sector, and the Internet of Things will be the three major technology areas that will produce a significant impact as early as the coming year 2017 (1).
Predictive analytics is being used by hospitals and other leading healthcare organizations, for identification activities and patient risk stratification in relation to a number of chronic and acute conditions, including hepatitis C, sepsis, suicide risks mental health, medication adherence, diabetes, among others.
On the other hand, the proliferation of tools and wearables devices and overall connected devices, such as fitness monitors, mobile health applications, scales to measure weight, glucose monitors or blood pressure, among others, allows patients an unprecedented degree of flexibility when it comes to the management and control of their own health.
If we apply predictive analytics to all this immense volume of data generate and provide by the patients themselves, with the data already available in the hospital’s electronic health records, along with other external data generated by the surroundings, hospitals could make real analytical programs to help build loyalty, retain and manage patient health, and analyze the health context of the population they serve, with a broader and richer modern vision, a concept that is gaining more weight within the strategic initiatives of hospitals (population health management).
However, it is important to note that without interoperability standards, data governance models, and especially without a comprehensive digital strategy, the immense amount of information being generated becomes simply unmanageable and investments in this area will not have the return expected by the administrators.
A Conceptual Framework for the Digital Transformation of Hospitals
In order to define a digital strategy, it is essential to have a complete view of the challenges we face in the relationship with our patients (external view) and how we can satisfy them in the most efficient manner by adjusting the way we do things (inner vision). Without this comprehensive approach we run the serious risk of executing partial and/or disconnected actions.
Of course, any digital transformation initiative should not only be “aligned” with the strategy of the hospital, but also be immersed in and be part of it. Hospitals need to focus on the digital from the strategic perspective if they want to really be a lever for transformation and real changes and be a present and future leader. This is not a “technical problem”, but essentially a change in mindset.
To help healthcare organizations in this complex process, NTTDATA has conceptualized a framework that integrates different elements to be taken into account in the digital transformation of hospitals, with their interrelationships and dependencies. Using this, or any other existing conceptual framework on the market, can help organize the early stages of your work (2).
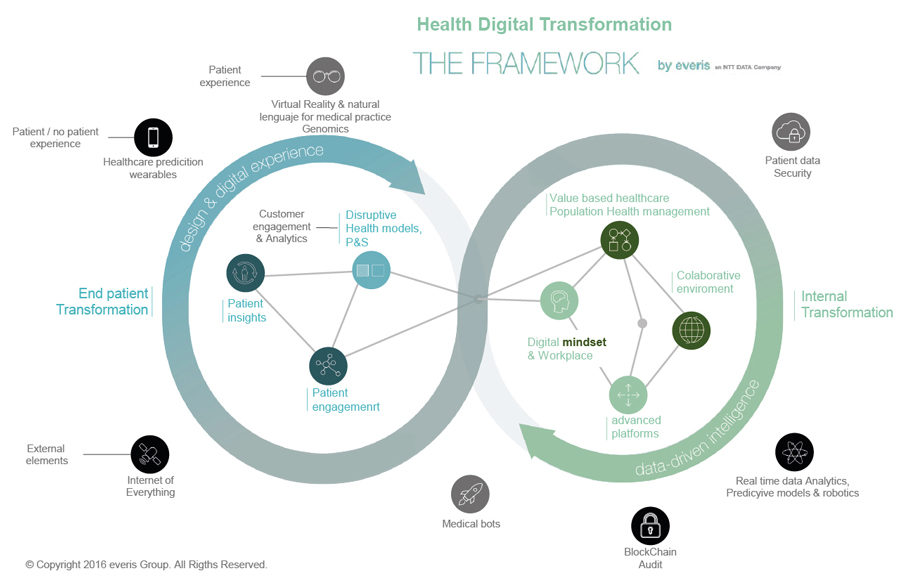
Hospitals in Latin America Face These Challenges
Finally, I would like to put forth some questions for those of us who work in the Latin American hospital sector. Are we prepared for this era of transformations? Will this be yet another moment in the social, economic and technological history of the region that we do not seize the opportunity to re-think ourselves and we settle for being spectators or, at best “reproduce” what others are doing without adapting it to our reality? In short, will we be true agents of change?
As we have seen, this is not just about modernizing infrastructure or medical technology. Above all, we need a change of mindset, a profound cultural change. Some hospitals in the region are in perfect condition to define their own way of transformation, aligned with the best global trends, but adapted to local circumstances. Others will continue thinking that it is a passing fad.
Public hospitals in turn, require the push and conviction of their governments, which must understand that the sustainability of the healthcare system in their countries depends largely on the degree to which they embrace these changes.
Ultimately, the hospitals that will emerge as future leaders will not be the ones with the highest billing rates or the best EBIDTDA ratios, but the ones that can best interpret the social, economic and current technological moment.
(2) Only some of these elements have been treated in this article for reasons of length
.png)




